How Does a Temporal Artery Temperature Reading Compared With an Oral Body Temperature Reading
- Research article
- Open up Access
- Published:
A comparison of temporal artery thermometers with internal blood monitors to measure trunk temperature during hemodialysis
BMC Nephrology volume 19, Article number:137 (2018) Cite this article
Abstruse
Background
Thermometers that measure cadre (internal) body temperature are the aureate standard for monitoring temperature. Despite that almost mod hemodialysis machines are equipped with an internal blood monitor that measures core torso temperature, current practice is to use peripheral thermometers. A better understanding of how peripheral thermometers compare with the dialysis machine thermometer may assistance guide practise.
Methods
The report followed a prospective cross-sectional design. Hemodialysis patients were recruited from 2 sites in Calgary, Alberta (April – June 2017). Torso temperatures were obtained from peripheral (temporal artery) and dialysis machine thermometers meantime. Paired t-tests, Banal-Altman plots, and quantile-quantile plots were used to compare measurements from the 2 devices and to explore potential factors affecting temperature in hemodialysis patients.
Results
The mean body temperature of 94 hemodialysis patients measured using the temporal avenue thermometer (36.7 °C) was significantly different than the dialysis auto thermometer (36.iv °C); p < 0.001. The mean difference (0.27 °C) appeared to be consistent across boilerplate temperature (range: 35.eight–37.three °C).
Conclusions
Temperature measured by the temporal artery thermometer was statistically and clinically college than that measured by the dialysis machine thermometer. Using the dialysis machine to monitor trunk temperature may issue in more authentic readings and is probable to reduce the purchasing and maintenance costs associated with manual temperature readings, as well equally easing the workload for dialysis staff.
Groundwork
Measuring pre-dialysis body temperature is a routine function of intendance in many hemodialysis (Hard disk) units. Although the gilded standard for body temperature measurement is the temperature of central (cadre) blood, measurements of this parameter are not bachelor in nigh clinical settings, and and so temperature is typically measured at other sites, such as oral, axillary, tympanic, or temporal artery.
Modern HD machines are ofttimes equipped with an internal blood temperature monitor that tin display core temperature readings. Despite this, common practice in many units is to record manual temperatures using peripheral thermometers. This practice is potentially unnecessary and may introduce fault, given the known inaccuracy of peripheral temperature measurement [i].
In this written report, we compared trunk temperature measured by HD machine thermometers with those measured by temporal artery (TA) thermometers. Our secondary objective was to appraise the feasibility of replacing the currently used TA method with dialysis machine (DM) thermometers.
Methods
Written report design
This prospective cantankerous-sectional study is presented co-ordinate to the STROBE guidelines for cross-sectional studies [2]. This study was approved past the Academy of Calgary Conjoint Ethics Board.
Eligibility criteria
All adult (≥ 18 years) patients with a diagnosis of cease-stage renal disease, currently undergoing hemodialysis for at least ane month at one of the two study sites in Calgary, Alberta, and able to provide informed consent were invited to participate. Patients were recruited betwixt April and June 2017.
Outcomes
The main event of the report was body temperature (°C). Other outcomes of interest were whether mean temperature varied depending on certain patient characteristics (cocky-reported gender, age, years on dialysis, diabetes, etc.) and thermometer preference of patients and nurses.
Data drove
All patients treated in Calgary hemodialysis units are dialyzed using the Fresenius 5008 auto. This automobile is equipped with an internal claret monitor that measures arterial temperature to ii decimal places, which is transmitted to each unit's electronic medical record system. Electric current practice locally is to monitor the patients' temperature using a TA thermometer (Exergen Corporation, Massachusetts/United states of america). This device uses infrared technology to measure temporal avenue temperature to 1 decimal identify. Dialysis nurses and nurses' aides collected the temperatures at the outset of dialysis treatment on a all-time efforts basis. In some cases, temperature was collected afterward in the treatment, which was recorded as such. All data was collected during a single dialysis session per patient. Nurses or aides measured body temperature with the TA and DM methods simultaneously. Three measurements were taken for each method, 1 min apart (a total of 6 measurements). Participants were asked whether they preferred to have their temperature measured by the peripheral thermometer or directly by the Hard disk machine. Nurses were also asked to submit anonymous surveys to the research administration describing their preferences and willingness to use the dialysis automobile reading.
Sample size calculation
A sample size adding indicated that xc patients would be required to yield 80% ability to demonstrate a 0.3 °C deviation between thermometer method pairs, assuming blastoff = 0.05. The standard difference of the difference between methods was assumed to exist 1 °C, consequent with prior literature [3,4,5].
Statistical methods
The mean difference and the 95% conviction interval (CI) of the two thermometer types (TA - DM) were calculated. In the principal analysis, nosotros used the first pair of temperature measurements from each patient (one temperature using TA and ane using DM), regardless of the fourth dimension at which those measurements were made. A paired t-test was used to test the temperatures of each thermometer type. A Bland-Altman plot [half dozen] was created to appraise the level of understanding. Because dialysis treatment might modify body temperature, we also did a sensitivity analysis including just pairs of first temperatures that were obtained during the first xv min of treatment initiation. We did a 2nd sensitivity analysis that compared the mean value of the three temperatures within the get-go 15 min of handling by each method (TA and DM).
Temperatures were compared between groups using t-tests (dichotomous variables) or ANOVA (categorical variables). A quantile-quantile plot was used to compare the distribution of temperature betwixt thermometers.
Results
Demographics
In total, 94 patients provided consent and all were included in the analysis (Table i). Over half (59%) were male, the hateful ± SD historic period was 65 ± thirteen.six years, and the median number of years since dialysis initiation was iv years (Table ane). Body temperature was measured during the first 15 min of the Hard disk handling in 87 patients (92.6%). Hateful temperatures among HD patients were 36.4 °C by the HD machine and 36.7 °C by the temporal artery thermometer.
Temperatures as measured by temporal artery versus HD motorcar thermometers
The distribution of the TA and DM measurements were both normally distributed (Fig. 1). The mean temperature measured by the TA thermometer was 36.7 °C (Table 2), which was significantly different (p < 0.001) than the hateful DM temperature of 36.42 °C (Fig. 1). The mean difference (95% CI) between the TA and DM temperature was 0.27 °C (0.xviii–0.37). The Banal-Altman test for understanding showed that 3/94 observations were outside the limits of 95% agreement (Fig. 2). Nosotros institute that 2/94 (2.1%) patients had temperatures below 36 °C using the TA thermometers, compared to 12 (12.8%) using the dialysis machine thermometer.
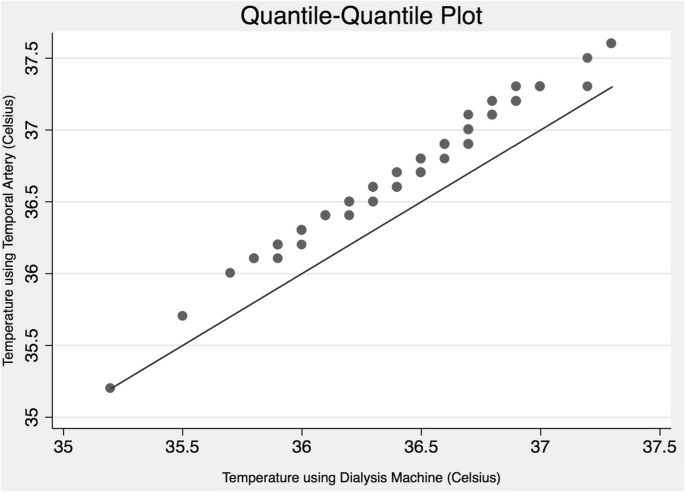
Quantile-quantile (Q-Q) plot comparing the distribution of body temperature of hemodialysis patients, measured past a temporal artery thermometer and an internal blood monitor of the dialysis machine. This plot assesses whether the distribution of temperatures are equal between the ii thermometer methods (using the first temperature reading of each device simply). Every bit the temporal artery values are all consistently in a higher place the reference line, this Q-Q plot suggests a higher temperature when using the temporal avenue thermometer, compared to the dialysis machine thermometer. Temperatures measured using the dialysis auto were rounded to single digit
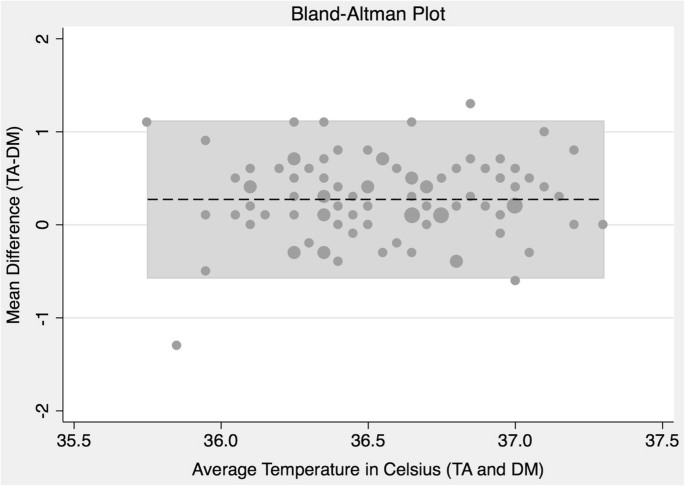
Bland-Altman Plot showing level of agreement betwixt the temporal artery (TA) and dialysis automobile (DM) thermometers. Of the 94 data points, 3 (3.2%) are outside the limits of agreement (− 0.57 and 1.12 °C). The mean divergence (dotted line) is 0.27 °C and is consequent over the boilerplate temperatures obtained in this study. Temperatures measured using the dialysis motorcar were rounded to unmarried digit. Larger points represent multiple patients with identical values
Sensitivity analysis
Results were similar in the sensitivity assay that compared only the get-go pairs of temperature measurement within the get-go 15 min of treatment (36.vii °C and 36.42 °C for TA and DM respectively, p < 0.001) (Table ii). Results were also similar in the 2d sensitivity assay, which compared the mean of the first three measurements inside the commencement 15 min of treatment (36.7 °C and 36.49 °C respectively, p < 0.001) (Table 2).
Preferences of patients and nurses
The large majority (95%) of patients did not express a preference well-nigh the thermometer type. Of the 12 nurses that completed a survey, 75% (n = 9) preferred using the dialysis machine instead of the brow thermometer to measure patient body temperature. Reasons given for this included increased convenience and accurateness, reduced workload, and less perceived risk of transmitting infection betwixt patients using the TA thermometer.
Epidemiology of body temperature amid Hard disk drive patients
There was no evidence that torso temperature amidst HD patients statistically differed past the time of 24-hour interval. For example, median temperatures every bit measured by the Hard disk machine were 36.24 °C during shift 1, 36.44 °C during shift 2, and 36.50 °C during shift 3) (p = 0.53). We as well found no meaning differences in median body temperature past gender (36.40 °C in males, 36.44 °C females; p = 0.68), age (36.49 °C in patients less than 65 and 36.36 in patients ≥65 years, p = 0.15), or years on dialysis (36.43 °C if < vi years, 36.40 °C if ≥6 years, p = 0.72). The temperature of patients with diabetes (36.33 °C) was significantly lower than those without (36.52 °C) p = 0.02.
Discussion
We plant a statistically pregnant difference between trunk temperatures measured using temporal artery thermometers and core blood temperature measured by the dialysis machines. The mean difference between the methods was 0.27 °C, with the TA device reporting college temperatures than the DM method. If 1 considers the DM method to be the golden standard, the limits of agreement (1.69 °C) exceed the recommended clinically acceptable difference of 0.5 [7], suggesting that the TA device may non exist platonic for routine clinical use, given that a superior measurement is readily available.
To our knowledge, this is the outset study comparing methods of temperature measurement in HD patients. Studies done in other populations have also reported a departure between temperatures measured using peripheral thermometers compared to those measuring core temperatures [1], [viii,9,x]. A meta-analysis of hateful differences in afebrile patients reported that temporal avenue thermometers were 0.07 °C higher than the reference core temperature [8]. Even so, this analysis included children and adults and a variety of core thermometer types, which could explicate the lower discrepancy than found in our written report. Interestingly, the meta-analysis found that TA thermometers underestimated temperatures amidst febrile patients (hateful difference of − 0.19 °C). Taken together with our findings (overestimation of temperature among HD patients), these findings suggest that the temperatures obtained using TA thermometers may bias towards the mean ("normal") temperature every bit seen in healthy populations. However, since all of the Hard disk drive patients we studied were afebrile, this suggestion is speculative.
We found no association between torso temperature and factors such as age, gender, years on dialysis, or time of mean solar day. This finding contrasts with previous research that showed a pregnant difference past gender [11] and fourth dimension of 24-hour interval [12] in good for you individuals. Possible explanations for the discrepant finding could be related to kidney failure or because the participants in this study were older (IQR: 56–75 years). Patients with diabetes had significantly lower body temperature than those without, although the magnitude of the difference was modest.
The findings from this written report have potential implications for clinical do. Considering core temperature as the gold standard, the temperatures measured by the dialysis machine thermometer were statistically dissimilar from those measured past the temporal artery thermometers. Although the magnitude of the difference was small, it might be clinically relevant in some scenarios. In addition, recording temperature from the dialysis machine may salve small amounts of staff fourth dimension compared to measuring it with a thermometer, peculiarly if the data can be captured automatically by linkage between the dialysis automobile and an electronic health tape. In our written report, although patients did not have a preference, most nurses preferred to measure temperature using the dialysis car.
While this study accomplished 80% ability, included a representative HD population, and collected temperature measurements using ii clinically relevant methods, it too has potential limitations. Kickoff, different nurses were involved in the data collection. Due to possible varying techniques, this could touch the precision of the temporal artery thermometers. However, this reflects real-world clinical do and therefore is appropriate for understanding the practical implications of this study. Secondly, while we aimed to always obtain the pair of study measurements inside the outset 15 min of treatment initiation, this was non possible in 7 of 94 patients. Results were similar in our sensitivity analysis (washed simply in patients whose measurement was made within the outset 15 min of treatment), suggesting that inclusion of these vii patients did not affect our results. I could debate that a more than stringent requirement (due east.g. making all measurements inside the showtime 30 s of dialysis) would have been preferable. However, although dialysis treatment may change truthful torso temperature, there is no potent reason to think that it should differentially bear on the temperature as measured by one technique vs. another. Even so, this is a potential limitation of our report. Thirdly, these findings may not be generalizable to patients with significant access recirculation, which may touch the accuracy of cadre temperature measurement past the DM method. Furthermore, dialysate temperatures were not monitored in this written report, which may have potential to influence the differences between the ii thermometer types. However, these are unlikely to have affected our primary conclusions. Finally, no febrile patients were included in this study and therefore the diagnostic performance of the two methods for detecting fever could non be compared.
Conclusions
The mean body temperature of hemodialysis patients as measured by a temporal artery thermometer was 0.27 °C college than the mean core temperature measured by the dialysis automobile. As core temperature is the gold standard, using the dialysis machine to measure body temperature in Hard disk drive patients rather than an external thermometer may result in slightly greater accurateness while possibly also lowering staff workload.
References
-
Niven DJ, Gaudet JE, Laupland KB, Mrklas KJ, Roberts DJ, Stelfox HT. Accuracy of peripheral thermometers for estimating temperature: a systematic review and meta-analysis. Ann Intern Med. 2015;163:768–77.
-
Found of Social and Preventive Medicine (ISPM) - university of Bern. STROBE: Strengthening the reporting of observational studies in epidemiology 2009 https://www.strobe-statement.org/index.php?id=strobe-home. Accessed: 08 Nov 2017.
-
Greenes DS, Fleisher GR. Accuracy of a noninvasive temporal artery thermometer for use in infants. Arch Pediatr Adolesc Med. 2001;155:376–81.
-
Hebbar Chiliad, Fortenberry J, Rogers K, Merritt R, Easley K. Comparison of temporal artery thermometer to standard temperature measurements in pediatric intensive care unit patients. Pediatr Crit Care Med. 2005;6:557–61.
-
Roy S, Powell K, Gerson LW. Temporal avenue temperature measurements in healthy infants, children, and adolescents. Clin Pediatr. 2003;42:433–7.
-
Bland JM, Altman DG. Measuring agreement in method comparison studies. Stat Methods Med Res. 1999;viii:135–sixty.
-
Hernandez JM, Upadhye S. Do peripheral thermometers accurately correlate to Cadre body temperature? Ann Emerg Med. 2016;68:562–3.
-
Geijer H, Udumyan R, Lohse Grand, Nilsagard Y. Temperature measurements with a temporal scanner: systematic review and meta-analysis. BMJ Open. 2016;6:e009509.
-
Kiekkas P, Stefanopoulos N, Bakalis N, Kefaliakos A, Karanikolas M. Agreement of infrared temporal artery thermometry with other thermometry methods in adults: systematic review. J Clin Nurs. 2016;25:894–905.
-
Kimberger O, Cohen D, Illievich U, Lenhardt R. Temporal avenue versus bladder thermometry during perioperative and intensive intendance unit monitoring. Anesth Analg. 2007;105:1042–7.
-
Mackowiak PA, Wasserman SS, Levine MM. A critical appraisal of 98.6 degrees F, the upper limit of the normal body temperature, and other legacies of Carl Reinhold August Wunderlich. JAMA. 1992;268:1578–80.
-
Usvyat LA, Kotanko P, van der Sande FM, Kooman JP, Carter One thousand, Leunissen KML, Levin NW. Circadian variations in trunk temperature during dialysis. Nephrol Punch Transplant. 2012;27:1139–44.
Acknowledgements
The authors thank the patients involved in this written report and the dialysis heart staff for their assistance in collecting the data for this report.
Availability of information and materials
The data that support the findings of this study are available from Alberta Health Services only restrictions apply to the availability of these data, which were used under license for the electric current study, and and then are non publicly available. Information are however bachelor from the authors upon reasonable request according to the terms of relevant Alberta privacy legislation and regulation.
Author information
Affiliations
Contributions
ML, RL, JM, and MT contributed to the conception or design; ML and BT acquired the data; ML, BT, NW, CT, and MT contributed to the assay and interpretation of data; and ML and MT drafted the manuscript. All authors provided intellectual content of disquisitional importance and approved the terminal version.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This written report was approved past the University of Calgary Conjoint Ethics Board. All participants provided written informed consent.
Competing interests
The authors declare that they take no competing interests.
Publisher'due south Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed nether the terms of the Creative Commons Attribution iv.0 International License (http://creativecommons.org/licenses/past/4.0/), which permits unrestricted use, distribution, and reproduction in whatsoever medium, provided y'all give advisable credit to the original writer(south) and the source, provide a link to the Creative Commons license, and signal if changes were made. The Creative Eatables Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made bachelor in this article, unless otherwise stated.
Reprints and Permissions
About this article
Cite this article
Lunney, M., Tonelli, B., Lewis, R. et al. A comparison of temporal artery thermometers with internal blood monitors to measure torso temperature during hemodialysis. BMC Nephrol xix, 137 (2018). https://doi.org/10.1186/s12882-018-0938-x
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1186/s12882-018-0938-x
Keywords
- Temperature
- Thermometer
- Hemodialysis
- Banal-Altman
Source: https://bmcnephrol.biomedcentral.com/articles/10.1186/s12882-018-0938-x
Postar um comentário for "How Does a Temporal Artery Temperature Reading Compared With an Oral Body Temperature Reading"